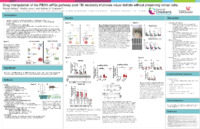
Examining Drug Intervention on Stress Responses After Traumatic Brain Injury
Main Article Content
Abstract
By Rohan Bellary, Medical Sciences
Advisor: Shelby Hetzer
Presentation ID: 222
Abstract: Traumatic brain injury (TBI) is known to cause primary physical symptoms as well as long-term secondary cellular responses. Traumatic optic neuropathy (TON) refers specifically to the optic nerve injury that can occur with TBI. TON leads to prolonged visual defects, including deficits in the optokinetic response (OKR) - the involuntary visual acuity response. Our lab has shown that TBI-induced TON leads to the activation of the Endoplasmic Reticulum (ER) stress response with specific activation of the PERK-eIF2a arm. TON-induced phosphorylation of eIF2a, a downstream elongation factor, can lead to the generation of apoptotic factors once phosphorylated or activate the cells unfolded protein response. Researchers now ask whether continued phosphorylation of eIF2a leads to an apoptotic response and reduction of an adaptive response, or vice versa. Post closed head TBI adult mice were injected with Salubrinal (increases p-eIF2a), ISRIB (decreases p-eIF2a), or vehicle 60 minutes post-injury then OKR was tested over 4 days. OKR analysis showed Salubrinal improved visual response while ISRIB improved visual acuity in TBI mice. Western blot analysis of retinal tissue revealed an increased ratio of p-eIF2a/eIF2a in TBI+Salubrinal mice compared to ISRIB. RBPMS - a measure of retinal ganglion cells- was found to be decreased in all TBI conditions, indicating that neither drug provided RGC saving functions. Data showed that drugs were beneficial in improving overall visual functioning in TBI conditions, however further studies need to be completed to fully understand the effects on adaptive vs. apoptotic cellular responses.